Proximal Humerus Fracture
By Nigel ChuaProximal humeral (humerus) fractures happen when the top aspect of the upper arm bone, that is shaped like a ball, is fractured or has a break.
They are also commonly called shoulder fractures, which are categorized and grouped according to
- the location of break on the humeral bone
- how many pieces it broke into (2, 3, 4 or more pieces)
- whether the shoulder humeral fracture includes movement (translation and/or dislocation).
The most common causes of proximal humerus fractures are falling onto an outstretched hand, or being involved in a road traffic or motor vehicle accident which includes high force or speed.
The good news is that most of the time, proximal humeral fractures do not require any corrective surgical operations. They are usually treated with immobilization and rest in a sling, followed by shoulder fracture rehabilitation to improve shoulder movement and strength.
HUMERUS BONE REVIEW
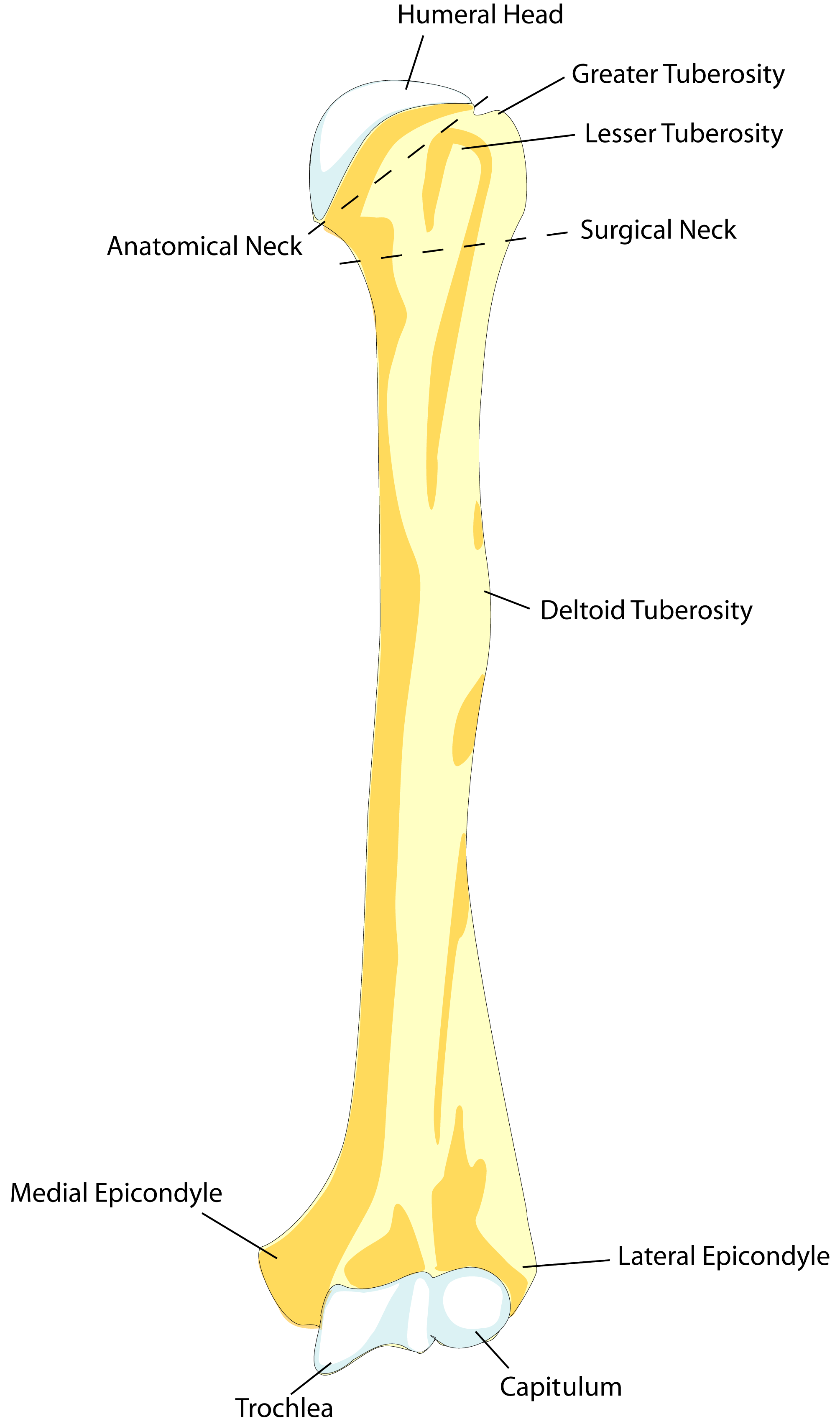
Our humerus/humeral bone refers to the long bone in our upper arm that sits between our shoulder and elbow, and the very top part of it is called the proximal humerus.
Proximal is a medical and anatomical term meaning "nearer to midline" - so in this case, the proximal humerus means the part of humerus that is closest to our midline, which is essentially the humeral head.
We have four rotator cuff muscles which attach to the humerus head, and they are the main muscles responsible for shoulder movement, stability and strength. Whenever our rotator cuff muscles or tendons are injured, it leads to difficulties and pain.
Here are the most important components to our proximal humeral bone:
Humeral Head
The top of the humerus is shaped like a ball (if you make a fist with your hand and then flex your wrist - that's very similar to how it looks and feels) and it is known as the head of humerus or humeral head.
Our humeral head rests in a fairly shallow socket that is formed by part of the shoulder blade, known as the glenoid fossa, to form the glenohumeral joint which is our shoulder joint.
Greater Tubercle/Tuberosity
Our greater tubercle refers to a large nodule (pure mass of bone) found on the outward facing side of the proximal humerus. Three of the four rotator cuff attach to the greater tubercle:
- supraspinatus
- infraspinatus
- teres minor.
Lesser Tubercle/Tuberosity
The lesser tubercle of the humerus refers to a smaller nodule which is found on the front side of the proximal humerus. The fourth rotator cuff muscle, called the subscapularis, attaches here.
Anatomical Neck
The anatomical neck of the humerus is a diagonal groove that is located between the head of humerus and the greater and lesser tubercles. The articular capsule of the shoulder joint attaches here.
Surgical Neck
The surgical neck of our humeral bone runs horizontally (straight across), just below the greater and lesser tubercles at the bottom of the humeral head. Most proximal humerus fractures typically happen at the surgical neck.
WHAT ARE THE TYPICAL CAUSES OF PROXIMAL HUMERUS FRACTURES?
Proximal humerus fractures account for a large majority of fractures of the upper arm, and account for 5% of all fractures.
The most common causes of a proximal humerus fracture include:
Falls
As mentioned earlier, the most common cause of a proximal humerus fracture is falling over onto an outstretched hand (this is often abbreviated to "FOOSH").

In fact, what patients need to know is that the force or fall doesn’t need to be from any great height; falling from a standing height can be enough to break the proximal humeral bone.
A Direct Blow
A high-energy blow to the shoulder, such as
- a sports injury, e.g. a sporting tackle or collision
- a road traffic accident/motor vehicle accident
can also cause a proximal humerus fracture. Often in these high speed or power circumstances our shoulder joint can also dislocate, meaning that the head of humerus slips out of the glenoid socket.
Older Age
Approximately 75% of proximal humerus fractures occur in people over the age of 60 because our bones get weaker and more brittle with age, making them more likely to break and fracture.
Fractures of the proximal humerus are the third most common type of broken bone in the 65s age group, after hip fractures and wrist fractures.
Osteoporosis
With osteoporosis the bone becomes increasingly brittle and weakens, making it more likely to break. A milder version of this is low bone mineral density (osteopenia) which also increases fracture risks.
Gender
Women are three times more likely to experience a proximal humeral fracture than men - this could be due to variable factors such as:
- muscle strength and size to absorb force
- higher risk of osteoporosis or osteopenia
- balance issues.
CLASSIFICATION OF HUMERUS FRACTURES
A proximal humerus fracture is typically categorised using the Neer System which takes into consideration
- the number of fracture parts
- the level of “displacement” of these fractured humeral parts.
Neer divides the proximal humerus into four parts:
- The anatomical neck
- The greater tuberosity
- The lesser tuberosity
- The surgical neck
Neer then looks at the level of displacement of the parts - if there is more than 1cm of separation or the angulation is greater than 45 degrees, it is considered a displaced fracture.
One-Part Fractures
A one-part proximal humerus fracture means that there is no displacement.
Any one or more of the four parts may be fractured, but there is less than 1cm separation between the two fractured ends and less than 45 degree angulation.
For example there could be a fracture of the surgical neck and the greater tuberosity, but as long as neither of the parts are displaced, it is still classed as a one-part fracture.
Fortunately, most (up to 75%) of proximal humerus fractures are one-part fractures.
Two-Part Fractures
Two-part fractures occur when one part is displaced more than 1 cm or rotated more than 45 degrees. Again, there may be multiple fractures in multiple parts, but we're referring to at least one part being displaced.
Approximately 20% of proximal humerus fractures are two-part fractures.
Three-Part Fractures
Three-part fractures occur when two parts are displaced.
There will most likely be displacement of the surgical neck and one of the tuberosities (most of the time it involves the greater tubercle), while the other humeral tuberosity remains attached.
Approximately 5% are three-part fractures.
Four-Part Fractures
This occurs when all four parts are fractured, with three of them displaced in relation to the fourth.
Fortunately, a four-part fracture is very rare (less than 1% chance) but when it happens, it is classified as a very severe injury and almost always will require corrective shoulder surgery - patients are highly recommended for surgery unless medically not able to.
Fracture Dislocation
Fracture dislocations happen when the shoulder is dislocated with a proximal humeral fracture, meaning it has come out of its socket.
A proximal humerus fracture dislocation may be a two, three or four part fracture.
SYMPTOMS OF A PROXIMAL HUMERUS FRACTURE
Proximal humerus fractures don’t just happen without a form of external force, and most patients will be able to recall and connect the bone fracture to a specific event, date and place.
A proximal humerus fracture will typically cause:
- Pain: The pain from the shoulder injury and bone fracture will be near instant, severe and ongoing. Patients will know for sure that it is injured and possibly fractured.
- Limited Shoulder and Arm Movement: Patients will experience pain with any upper arm and shoulder movement (it will be extremely painful), so movement will be very restricted.
- Swelling and Bruising: There will be significant swelling and bruising in the upper arm which may extend all the way down to the hand within a couple of days of injury.
- Bony Sounds (Crepitus): Patients may be alarmed when they experience a grinding or grating noise or sensation when moving their broken humeral arm. These sounds and sensations are caused by the broken pieces of bone fragments rubbing against each other when moved.
- Obvious Fracture Deformity: If the patient's shoulder fracture is a displaced fracture, the arm may appear deformed or abnormal. If there is a fracture dislocation, the deformity will be obviously visible.
- Bleeding: If the fractured part has pierced or punctured the skin (termed as an open fracture) there will be bleeding.
- Altered Sensation: In some situations, the sharp bony fragments may injure the nerves around the shoulder and that may result in altered sensation, such as pins and needles or numbness below the fracture site. Less than half of all proximal humerus fractures have associated nerve damage, but it tends to be the axillary nerve that is most often affected.
DIAGNOSING HUMERAL FRACTURES
If our senior physiotherapists in Phoenix Rehab Singapore or your shoulder doctor suspects a proximal humerus fracture, you will be referred and sent for at least one type of imaging scan to evaluate the severity of the fracture, where exactly it is and how many parts, and if there is any dislocation or movement of the fractured parts.
Typically, taking x-rays with different angles of the shoulder and upper arm are enough to diagnose and categorize a humerus fracture.
X-rays are usually taken in three perpendicular planes:
- The front (true AP view)
- The side (lateral scapula Y view)
- Through the armpit (axillary view)
In some cases, you may also be sent for a CT or MRI scan if the x-ray imaging results aren't clear enough. If the greater tuberosity is fractured, an ultrasound scan will be performed to check for rotator cuff muscle and/or tendon damage.
TREATMENT OF A PROXIMAL HUMERUS FRACTURE
Conservative / Non-Operative Approach
The good news is that in most cases, a proximal humerus fracture will not require surgery. Nearly 80% of proximal humeral fractures are undisplaced or only minimal displaced fractures and therefore non-operative treatment is appropriate. Non-operative treatment for a proximal humerus fracture consists of:
1) Immobilization
For the first few weeks after a proximal humerus fracture, patients are required to keep their affected arm in a sling to hold the fracture still and to allow the swelling and pain to subside.
The shoulder fracture needs to be completely immobilized for at least 10-14 days to allow time for the bones to start slowly joining back together and heal, so the sling must be worn at all times.
After this, you can gradually reduce how much you wear the sling, and by around 12 weeks you shouldn’t need it at all.
Most of the time, patients are prescribed a shoulder immobilizer or sling and swath. These are good because they provide support to the elbow and forearm and counteract the weight of the arm. The extra strap around the body helps to keep the upper arm immobilized.
In some cases, patients may be issued a collar and cuff instead. These provide less support but allow the weight of the arm to provide gentle traction which can help improve the alignment of the fracture.
2) Medication
Medication to relieve pain and inflammation will be prescribed by your doctor such as NSAIDS (non-steroidal anti-inflammatories) e.g ibuprofen or naproxen.
If you have an open fracture or surgery you will also be given antibiotics to reduce the risk of infection.
3) Exercises
For the first couple of weeks after a proximal humerus fracture, the shoulder should be immobilized in the sling, but please note that it is very important to do your elbow, wrist and finger exercises to prevent any stiffness or weakness.
It's extra painful to have stiffness in the elbows, wrists and fingers, as well as the shoulder stiffness post-fracture.
Typically, you're allowed to take your arm out of the sling to do these exercises.
These exercises should be started as soon as possible and be done at least 3 - 5 times a day, if not more. It is important to move the elbow, wrist and fingers through their full range of motion. Hand grips and balls are a great way to maintain strength.
After about two weeks, you should be able to start gentle exercises to get the shoulder moving, and our senior physiotherapists will work on a shoulder physiotherapy program together with you.
Pendulum exercises are the best place to start for regaining mobility. These are exercises where you use gravity to move the arm so your muscles don’t have to do anything, so as to ensure that your muscles don’t catch onto or pull on the fracture site.
After around three weeks, you can start active assisted exercises (AAROM) where you use your good arm or a bar/stick to support and move the broken arm. You may also be prescribed a shoulder pulley system to use.
In terms of strengthening, you will start with isometric exercises.
These are exercises where you push against resistance but without any arm or muscle movement - this is so you don’t aggravate the fracture site. You may be allowed to start these as soon as pain allows, or you may need to wait until the fracture has fully healed – you will have to check with your doctor or our senior physiotherapists.
After about 6 - 10 weeks the fracture parts should have united and you can move on to active mobility exercises and progressive strengthening exercises, which may include resistance band exercises to regain rotator cuff strength.
Shoulder physiotherapy will continue until you have regained full
- movement
- strength
- stability
in the shoulder and elbow.
You may need to keep doing exercises for up to 12 months to achieve this. Please note that unfortunately not everyone regains full range of movement after a proximal humerus fracture, and some people will have ongoing difficulty lifting their arm above head height (but we will always aim for 100% recovery of course).
It is very important to rigorously follow your shoulder physiotherapy exercise program and do your shoulder exercises daily to ensure you regain as much range of motion, flexibility and strength as possible.
Failure to do so will lead to reduced shoulder movement which will likely cause pain, discomfort and ultimately will affect function.
Your shoulder doctor will see you regularly and x-ray the shoulder periodically to check on the healing process. Everyone heals at different rates, so follow the guidance of your doctor or our senior physiotherapist as to when you can progress to the next stage of rehab.
Surgical Approach
Unfortunately around 15% of proximal humerus fractures tend to be displaced and require surgery.
In most cases, metalwork is used to realign and fix the bones. This is a temporary measure to hold things together to allow the bone time to heal, and these are not meant to be a permanent support structure. The metal work may be removed at a later date if it comes loose or causes any problems. If the bone fails to unite, then further surgery will be required.
There are a few different types of surgery for a proximal humerus fracture depending on the type of fracture and the individual’s functional needs.
Closed Reduction
A closed reduction is where a proximal humerus fracture is realigned under anaesthesia without having to open up the shoulder with a scalpel (typically termed as MUA = manipulation under anesthesia).
This may be all that is needed, but if the MUA realignment proves to be unstable, then the surgeon may use percutaneous pins or K-wires to hold the bone in position. These are inserted through the skin and into the bone at various angles to hold the fracture still.
In some cases, the ends of the pins or K-wires are left slightly exposed so they can easily be removed once callus formation has begun, however there are increased risks of infection and pin movement (termed as migration or displacement), so buried pins may be safer to be used instead.
A closed reduction is most commonly done for two-part surgical neck fractures.
ORIF (Open Reduction Internal Fixator)
ORIF is the abbreviation for open reduction internal fixation and is where the fracture is stabilized and fixed using a metal plate and screws.
The orthopedic surgeon will make an incision at the front or side of your shoulder. If there is any fracture displacement, then the fracture will be reduced (brought together and realigned).
A metal plate is then inserted and held in place by surgical screws above and below the fracture site to keep it stable and secure. After that, the incision is then closed with staples or sutures.
An ORIF is most commonly done on younger patients for two, three or four part fractures or when there is displacement of the greater tuberosity.
Intramedullary (IM) Nailing
A small anterolateral (front and side) incision is made through the skin and through all underlying soft tissues.
The orthopedist will then insert a rod-shaped nail into the hollow centre of the humerus bone, known as the medullary canal and held in place with surgical screws. This splints the fracture from the inside to hold it steady.
Intramedullary nails are typically selected for a two part or three part proximal humerus fracture, or if there is also damage to the humeral shaft below.
Shoulder Hemiarthroplasty
A shoulder hemiarthroplasty (partial shoulder replacement), involves removing the humeral head and replacing it with a metal implant.
The stem of the implant is inserted into the medullary canal (the hollow middle of the upper arm bone) and will either be wedged tightly in place or secured with special bone glue cement.
The shoulder head "ball" is then attached to the top of the stem.
Most of the time, a shoulder hemiarthroplasty is done where the fracture is especially complex or if other treatment methods have failed. This may occur with an anatomical neck fracture, a four-part fracture, a fracture dislocation, or if the rotator cuff has also been damaged.
If the blood supply to the humeral head has been compromised and there is a high risk of osteonecrosis (where the bone starts to rot and dies), your shoulder surgeon will likely refer a hemiarthroplasty to be the treatment of choice.
Total Shoulder Arthroplasty
A total shoulder arthroplasty is when both parts of the shoulder joint are replaced (the arm, and the body part where the arm attaches).
The ball-shaped humeral head is removed and replaced with a metal implant. The implant is shaped like a half moon and has a stem which runs down the middle of the humerus bone.
The socket part of the joint on the shoulder blade is shaved down and a plastic socket is positioned and held in place with special cement.
Shoulder replacement is not always the first option - it will be done only if there is damage to the shoulder blade socket (the glenoid) together with the proximal humerus fracture.
The glenoid fossa/process may have been damaged at the time of injury or there may be significant arthritis (wear-and-tear, degeneration) in the joint that would make a partial shoulder replacement unsuitable.
The rotator cuff muscles and tendons must be intact for a total shoulder arthroplasty, if not there is a high risk of loosening of the prosthesis.
93% of total shoulder replacements typically last at least 10 years.
Reverse Shoulder Replacement
If the patient's rotator cuff tendons have been damaged (partially torn or completely ruptured) with the proximal humerus fracture, then the shoulder surgeon may recommend a reverse shoulder replacement.
It is most suitable for people over the age of 70 who have low shoulder movement and strength needs.
One requirement is that the deltoid muscle of the shoulder must be functioning well, strong and in good working order.
In a reverse shoulder replacement,
- the ball part of the implant is placed on the shoulder blade
- the socket is placed on the humerus.
This is the opposite way round to normal - that's why it's called "reverse".
This may sound like a strange thing to do, but what it does is allow the deltoid muscle to make up for the deficiency in the rotator cuff to allow greater shoulder movement than would otherwise be possible.
RECOVERING FROM A PROXIMAL HUMERUS FRACTURE
The rehabilitation and recovery process following a proximal humerus fracture is basically the same whether the patient was treated with or without surgery. The most important part of the recovery process is improving and regaining the shoulder range of movement.
Phase 1: Weeks 0 - 4
During this phase, patients will have their affected shoulder and arm immobilized and protected in a sling, which needs to be worn all the time (yes, night and day) except when
- showering
- changing dressings
- doing exercises.
Patients will be taught a few exercises:
- shoulder pendulum exercises
- active range of motion exercises for unaffected joints (elbow, wrist, fingers etc).
Phase 2: Weeks 4 - 10
Patients will continue to review with their treating shoulder surgeon and x-rays will be done regularly. Once the fracture has started to unite with no dislocation or displacement, then we can up the exercises:
- actively-assisted shoulder exercises, and the amount of assistance and support is progressively weaned off
- the patient is allowed shoulder involvement for gentle functional movement and use, without pain.
Phase 3: Week 10 Onwards
At this stage, patients can progress to more "strong" strengthening exercises. We will often start with isometric strengthening and gradually progress to strengthening exercises with shoulder/arm movement. This will continue to progress until the patient has achieved 100% recovery in shoulder strength and mobility/movement
As a general guideline patients can expect:
- Week 1: to be able to write and type, use phone etc
- Week 6 - 12: for the bone to have fully healed and you should no longer need to use your sling
- Week 12 (3rd Month): to be able to reach up to get things from a cupboard and hang the washing on the line
- Week 12 - 24 (3 - 6 months): to get back to lifting without any restriction
- Week 26 to 52 (6 - 12 months): to have regained full function of the arm – shoulder mobility might always be partly restricted
On smoking:
Please note that research has shown that smoking (or using nicotine products) directly delays bone healing and can increase the risk of non-union by around 6 times (this is 600% increase of bone fracture issues).
Nicotine restricts the size of blood vessels by around 25% which means the bone gets less of the oxygen and nutrients it needs to heal, which can significantly slow down the healing process.
POTENTIAL COMPLICATIONS RELATED TO PROXIMAL HUMERUS FRACTURES
The most common complications that a patient may experience with a proximal humerus fracture injury include:
Decreased Shoulder Movement and Function
Full strength and mobility may never be achieved after a proximal humerus fracture, particularly in elderly patients or those who do not follow their shoulder physiotherapy exercise program.
Patients may take up to 12 months to regain their full shoulder movement and strength with shoulder physiotherapy.
Frozen Shoulder
Also known as adhesive capsulitis, frozen shoulder happens when our shoulder joint capsule thickens and tightens which can cause:
- shoulder pain
- very limited shoulder movement.
Most of the time, this can happen when the shoulder is not moved (immobilized or protected) for a long period of time. Starting a shoulder physiotherapy exercise program as early as possible helps to reduce the risk of developing a frozen shoulder.
Avascular Necrosis (AVN)
A proximal humerus fracture can disturb the blood supply to the humeral head, resulting in avascular necrosis aka osteonecrosis. Because of the impaired blood flow and supply to and from the humeral head, the bone cells gradually rot, wither and die.
The humeral head gradually collapses resulting in pain and reduced movement.
Blood flow to the humeral head comes from vessels that branch off the axillary artery and travel upwards from the armpit region. Anatomical neck fractures and four-part fractures are the most likely to impede blood flow and cause avascular necrosis.
Arthritis
Damage to the shoulder joint increases the risk of developing early shoulder osteoarthritis, which can be very painful and affects daily function.
Surgical Risks
Any surgery has the risk of
- infection
- nerve damage
- poor bone healing (e.g. non union, mal union)
- wound healing problems
- loosening of the prosthesis.
Reference Sources:
- https://www.shoulder-pain-explained.com/proximal-humerus-fracture.html
Browse other articles by category
Physiotherapy for Knee Pain Physiotherapy For Slipped Disc Physiotherapy for Neck Pain PHYSIOTHERAPY
PHYSIOTHERAPY
 Hand Therapy
Hand Therapy
 Alternative
Alternative
 Massage
Massage
 Traditional Chinese Medicine Treatment
Traditional Chinese Medicine Treatment
 Rehab
Rehab
 Physiotherapy For Lower Back Pain
Physiotherapy For Shoulder Pain
Orthopedic Doctors, Insurance & Healthcare
Physiotherapy For Upper Back Pain
Frozen Shoulder
Physiotherapy for Back Pain
Physiotherapy For Lower Back Pain
Physiotherapy For Shoulder Pain
Orthopedic Doctors, Insurance & Healthcare
Physiotherapy For Upper Back Pain
Frozen Shoulder
Physiotherapy for Back Pain
 Whatsapp us now
Whatsapp us now