Radio-humeral joint synovitis elbow pain physiotherapy
By Nigel ChuaWHAT IS RADIOHUMERAL SYNOVITIS?
Let’s first understand what radiohumeral means.
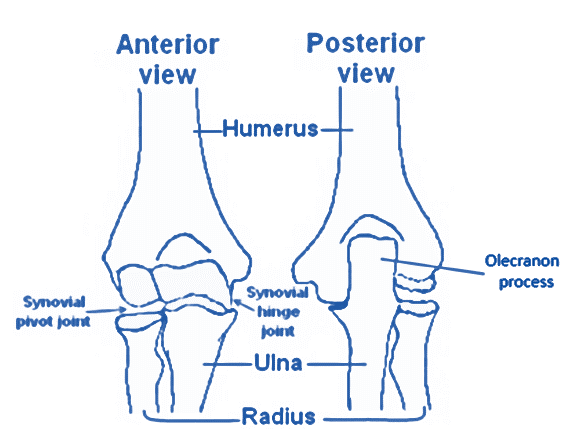
The radiohumeral joint is one of the three main joints in the elbow. It is situated between the radial head and the capitulum of the humerus. Part hinge and part ball-and-socket joint, the radiohumeral joint stabilizes and enables movement between the humerus and radius.
Now, synovitis is the medical term for the inflammation of the synovium.
The synovium, also called the synovial membrane, refers to the connective tissues that line the joint cavities (commonly known as synovial joints).
The purpose of this inner lining is to support and protect the joint during movement. It does this by secreting a viscous liquid, i.e. synovial fluid that acts as a lubricant and prevents damage to the joint cartilage due to friction.
Synovium is found in various joints in your body, including the
- knee
- ankle
- foot
- wrist
- hand
- shoulder
- elbow.
If it becomes inflamed due to any reason, it is known as synovitis.
Synovitis can make your joints ache, especially when you move them. The knees are usually more susceptible to synovitis, but it can occur in the elbow as well.
When the synovial lining becomes inflamed, it also irritates the surrounding nerves and tissues. This can make the joint swell and sensitive to touch. In most cases, synovitis can cause bleeding in the joint, which further aggravates the pain.
Untreated and prolonged synovitis can progress into soft tissue degeneration or, worse, bone loss.
Synovitis of the radiohumeral (RH) joint is a painful elbow condition marked by:
- Stiffness
- Swelling
- Redness
- Decreased joint mobility.
Synovitis usually develops in patients with arthritis, but there are several factors that can contribute to this type of joint pain.
In this article, we take a detailed look at what RH synovitis is. We discuss its symptoms, causes, treatment options, and how physiotherapy can help.
SIDE NOTE: SYNOVITIS VS. ARTHRITIS
Many people confuse synovitis with arthritis. While both of these conditions have to do with joint inflammation, they are actually different.
You can think of synovitis as a type of active inflammatory arthritis. Although arthritis affects joints, it does not always irritate the synovial membrane.
In other words, synovitis can occur in combination with arthritis and related conditions like gout and lupus, or simply on its own.
WHAT CAUSES SYNOVITIS OF THE RH JOINT?
Several factors can cause inflammation of the synovium in the radiohumeral joint.
They can be broadly classified into two main categories: structural damage and medical conditions that affect the synovial lining in joints.
When RH synovitis develops independently, it is usually due to structural damage, such as a labrum tear or ligament strain caused by direct trauma or joint overuse.
Medical conditions that can result in synovitis in the elbow include rheumatoid arthritis, osteoarthritis, systemic lupus erythematosus, and other auto-immune diseases wherein your body can mistakenly attack the joint lining.
The most common causes of RH synovitis typically include:
- Repetitive strain injury
- Arterial bleeds
- Overworking or overloading the elbow joint
- Previous hand or elbow injury
- Infections, such as tuberculosis, psoriatic or septic arthritis.
SYMPTOMS OF RADIOHUMERAL SYNOVITIS
The symptoms of elbow synovitis vary depending on the major cause of the inflammation. However, most people experience the following:
- Pain in the elbow – Ranging from mild to severe, the pain can be persistent or can come and go on its own.
- Swelling – Inflammation of the synovium leads to an increase in fluid production. With the buildup of synovial fluid, the tissues lining the joint become thickened, and your elbow becomes swollen.
- Redness and warmth – When the synovium is irritated, your body sends more blood to the affected area. This can give you a feeling of warmth or a tingling sensation in the joint. At times, there may be red patches on the skin resulting from internal bleeding. The elbow looks puffy and feels boggy to the touch.
- Loss of elbow joint movement or mobility – Synovitis can affect hand dexterity and grip strength. Patients may find it difficult to perform certain motions, such as pinching an object between their thumb and fingers.
- Increased body temperature – People with synovitis can develop a fever, especially when there’s an active bleed.
WHO IS AT RISK OF DEVELOPING ELBOW RADIO-HUMERAL SYNOVITIS?
RH synovitis is common in older adults, particularly if they have arthritis.
This condition is also associated with some specific sporting activities that involve excessive flexion and extension of the elbow, for example
- golf
- tennis
- badminton
- volleyball.
According to medical research, certain factors can increase your risk of developing synovitis.
These include:
- Gender – Women are generally more likely to develop synovitis than men.
- Age – Synovitis can occur at any age, but people above the age of 40 years are usually more susceptible to this disease.
- Genetics – If someone in your family has synovitis or any kind of arthritis, it increases your chances of developing this problem too.
- Smoking – In many cases, an association between smoking and synovitis has been observed.
- Obesity – People who are overweight or eat a lot of junk food may be at a higher risk of experiencing synovium inflammation.
OTHER CONDITIONS THAT ARE SIMILAR TO SYNOVITIS OF THE RH JOINT
Elbow pain due to radiohumeral synovitis can be confused with many other lateral elbow conditions, such as:
- Radiohumeral bursitis
- Osteochondritis dissecans in the elbow joint
- Carpal tunnel syndrome
- Radial tunnel syndrome
- Tennis elbow.
Hand dexterity or reduced joint mobility due to radiohumeral synovitis can also mimic the symptoms of osteoporosis and rheumatoid nodules.
Joint bleeds in the elbow are usually the primary pointers of synovitis of the RH joint.
However, arterial bleeding in the synovium is not a common symptom and occurs in extreme cases only.
TREATMENT OF RADIOHUMERAL SYNOVITIS
Synovitis that occurs due to physical damage to the joint can sometimes go away on its own. However, if the symptoms persist, treatment must be expedited.
The underlying cause of the inflammation dictates the treatment plan for this condition.
Medical Scans
The treatment for radiohumeral synovitis typically begins with diagnostic tests. Your doctor will aim to identify the cause of the pain by first determining whether or not it is true synovitis.
True synovitis means the symptoms are actually caused by inflammation of the synovial membrane. At times, inflammation of the surrounding joint tissues can imitate the signs of RH synovitis. The correct medical term for this condition is tendonitis.
Patients are often referred to get an x-ray of the elbow or undergo an MRI scan as it helps doctors rule out differential diagnoses and identify the extent of joint damage.
Synovial Fluid Analysis
The synovial fluid analysis helps determine if the inflammation might be caused by diseases like arthritis.
It takes about 30 minutes and requires no former preparations. The physician draws a sample of the joint fluid in the elbow and sends it for lab examination.
Medications
The treatment for radiohumeral synovitis commonly involves the administration of anti-inflammatory medications.
NSAIDs, such as aspirin and ibuprofen, are often injected directly in the affected area for targeted action. Sometimes, medicines for pain management might also include oral drugs called Disease-Modifying Anti-Rheumatic Drugs (DMARDs).
Although steroid injections are a popular method for controlling pain due to synovitis, they are not a cure.
Surgery
If conservative methods fail to bring relief, patients with synovitis might eventually have to consider surgical treatment.
This is referred to as a synovectomy and can be of two types:
- Arthroscopic synovectomy – Involves the removal of the inflamed part of the synovial membrane. This helps reduce joint bleeding and protects the elbow from degenerating.
- Radionuclide synovectomy – Here, a low-level radioactive substance is administered directly into the radiohumeral joint. The radiation gradually melts away the irritated membrane, preventing further synovium damage.
HOW PHOENIX REHAB HAND THERAPY AND PHYSIOTHERAPY CAN HELP PEOPLE WITH ELBOW RADIOHUMERAL SYNOVITIS
While it might not be possible to prevent synovitis, especially in patients with a known rheumatologic disease, it is, however, possible to slow it down.
Physiotherapy can have a beneficial effect, particularly in terms of alleviating pain, improving joint mobility, and increasing grip strength.
At Pheonix Rehab, we use special mobilization techniques in combination with conservative pain management methods to help our clients make a fast and effective recovery.
Our treatment for radiohumeral synovitis involves stretching and strengthening exercises that gradually restore healthy joint function in the elbow, wrist, and hands. Isometrics are often incorporated for their analgesic effect.
Physical therapy for synovitis typically utilizes an active range of pain-free movements to stimulate the production of healthy synovial fluid. Synovial fluid promotes the natural healing of the inflamed membrane, which, in turn, reduces pain and improves joint mobility.
Our qualified and trained physiotherapists in Phoenix Rehab Singapore perform a detailed assessment to figure out a comprehensive management strategy for synovitis. The overall treatment is geared towards controlling inflammation at the root, strengthening the joints and muscles, and increasing flexibility so that this condition doesn’t keep you from doing what you love.
Browse other articles by category
 PHYSIOTHERAPY
PHYSIOTHERAPY
 Hand Therapy
Hand Therapy
 Alternative
Alternative
 Massage
Massage
 Traditional Chinese Medicine Treatment
Traditional Chinese Medicine Treatment
 Rehab
Physiotherapy For Upper Back Pain
Physiotherapy For Shoulder Pain
Physiotherapy for Knee Pain
Physiotherapy For Slipped Disc
Orthopedic Doctors, Insurance & Healthcare
Rehab
Physiotherapy For Upper Back Pain
Physiotherapy For Shoulder Pain
Physiotherapy for Knee Pain
Physiotherapy For Slipped Disc
Orthopedic Doctors, Insurance & Healthcare
 Physiotherapy For Lower Back Pain
Physiotherapy for Neck Pain
Frozen Shoulder
Physiotherapy for Back Pain
Physiotherapy For Lower Back Pain
Physiotherapy for Neck Pain
Frozen Shoulder
Physiotherapy for Back Pain
 Whatsapp us now
Whatsapp us now