Regain vitality and live the pain-free life you deserve with Phoenix Rehab's physiotherapy treatments - no surgery or drugs required!
Experience the transformative power of physiotherapy – a science-based profession dedicated to enhancing your overall well-being.
Our skilled multi-disciplinary team of professionals is here to prevent, assess, and treat various movement disorders caused by physical disabilities, sports injuries, or illnesses.
Our personalised treatments relieve pain, improve muscle strength, enhance the joint range and mobility, boost exercise tolerance, and even aid chronic disease management.
Even better yet: At Phoenix Rehab, we go beyond just treating symptoms.
We take a holistic approach that considers you as a 'whole person', which includes considering your unique lifestyle factors and ensuring comprehensive care that nurtures your body, mind, and soul.
Don't let pain and limitations hold you back any longer!
Step into a world of renewed vitality and let our dedicated physiotherapy team guide you towards optimal health.
Tailored to Your Health Journey
Our Physiotherapy services
-
Muscle, Bone & Joint Pain Physiotherapy
-
Muscle, Bone & Joint Pain Physiotherapy
Common conditions we treat are Spinal Pain, Spinal Conditions, Headaches, Fractures, Joint Pain, Joint Stiffness, Joint Disorders, Muscle Tears, Dislocations, Sports Injury, and Hand Injuries.
Our goal is to provide the highest level of clinical rehab outcome while remaining professional and friendly, using evidence-based physiotherapy techniques and approaches in addition to exercise therapy.
Book an appointment today
-
Back Pain Physiotherapy
-
Back Pain Physiotherapy
Spine and back pain can be caused by various reasons or issues.
Still, most of the time, it's usually directly linked to trauma such as falls, direct blows/hits or motor vehicle accidents, poor posture, or repetitive strain injury.
Treatments by our specialist senior physiotherapists will help to decrease muscle spasms related to back pain, relieve spinal nerve root compression caused by slipped discs, and treat secondary conditions caused by compression of the sciatic nerve.
LEARN MORE Book an appointment today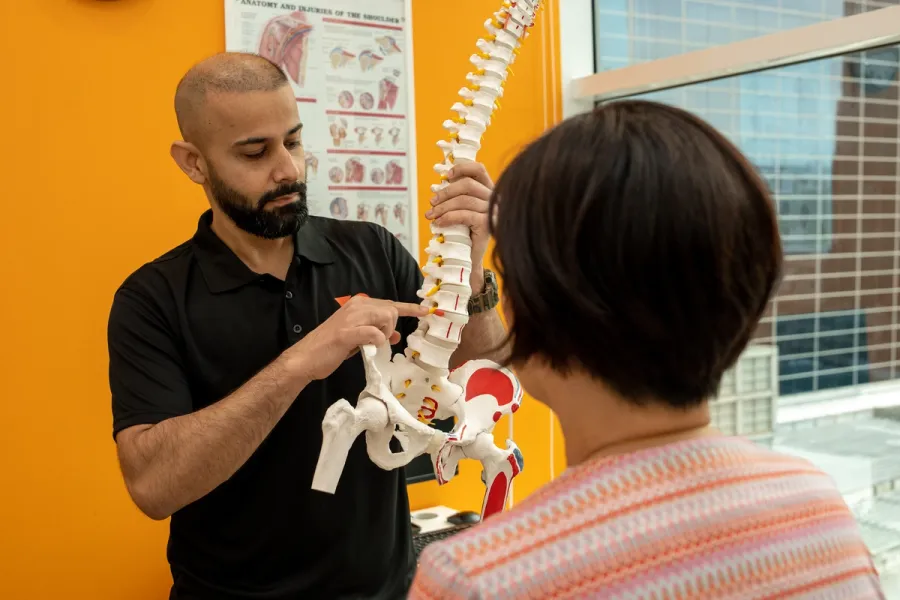
-
Neck Pain Physiotherapy
-
Neck Pain Physiotherapy
Our skilled therapists will diagnose and treat various conditions causing neck discomforts, such as muscle strains, cervical spine issues, and postural imbalances.
We'll help you treat pain, improve mobility, correct alignment, and restore your neck's natural strength through targeted exercises, manual therapy, and personalised care.
LEARN MORE Book an appointment today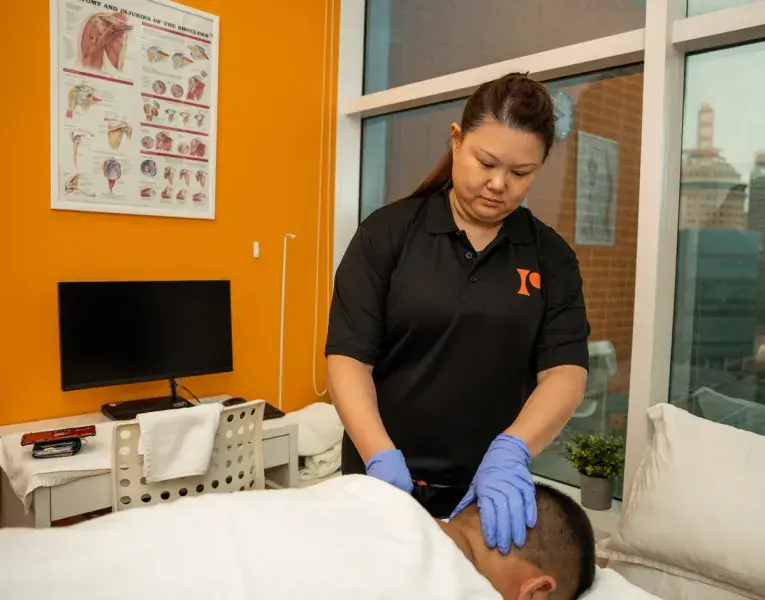
-
Shoulder Pain Physiotherapy
-
Shoulder Pain Physiotherapy
Our highly skilled therapists excel in diagnosing and treating various shoulder conditions, including rotator cuff tears, tendonitis, bursitis, and shoulder impingements.
Through targeted strengthening exercises, hands-on techniques, and tailored treatment plans, we provide efficient pain relief, enhance joint mobility, restore strength, promote healing, and optimise shoulder function.
LEARN MORE Book an appointment today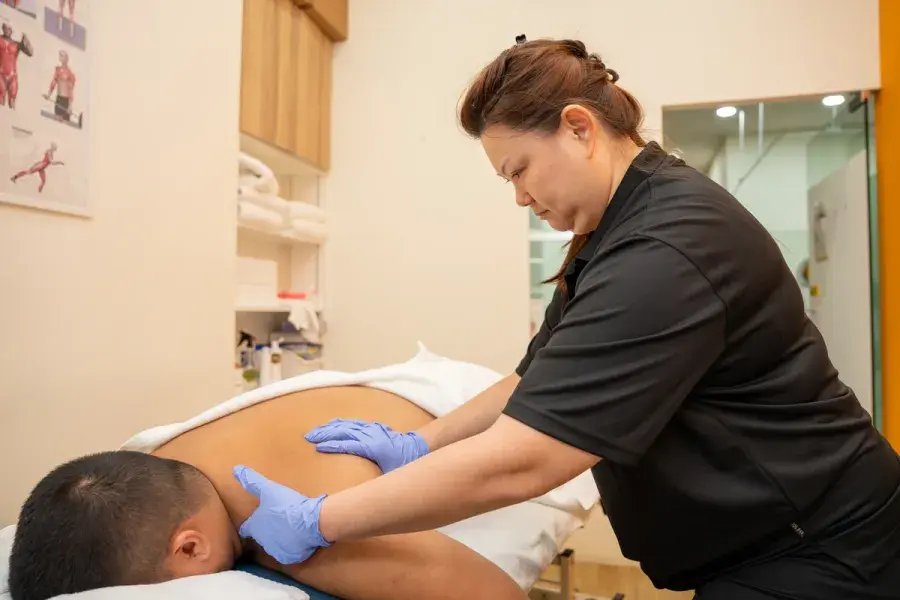
-
Frozen Shoulder Physiotherapy
-
Frozen Shoulder Physiotherapy
Frozen shoulder, medically known as adhesive capsulitis, is characterised by stiffness, pain, and limited mobility in the shoulder joint.
Our specialised physiotherapy treatment is designed to target and alleviate the root causes of frozen shoulder, allowing you to regain pain-free movement and reclaim your life.
LEARN MORE Book an appointment today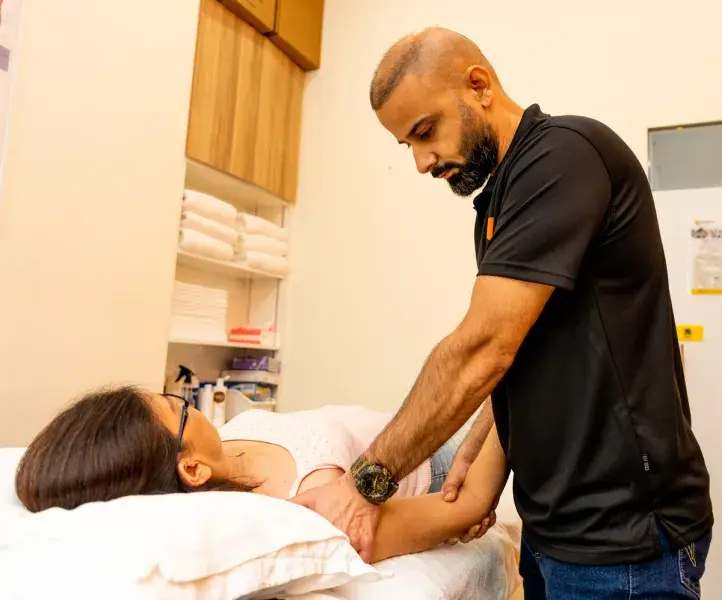
-
Hand Physiotherapy
-
Hand Physiotherapy
The hands are an essential part of our lives, enabling us to perform intricate tasks and express ourselves. Hand injuries, conditions, or surgeries can significantly impact our ability to function normally.
Luckily, our specialised hand physiotherapy treatment alleviates various hand-related concerns, facilitating a faster and more complete recovery.
LEARN MORE Book an appointment today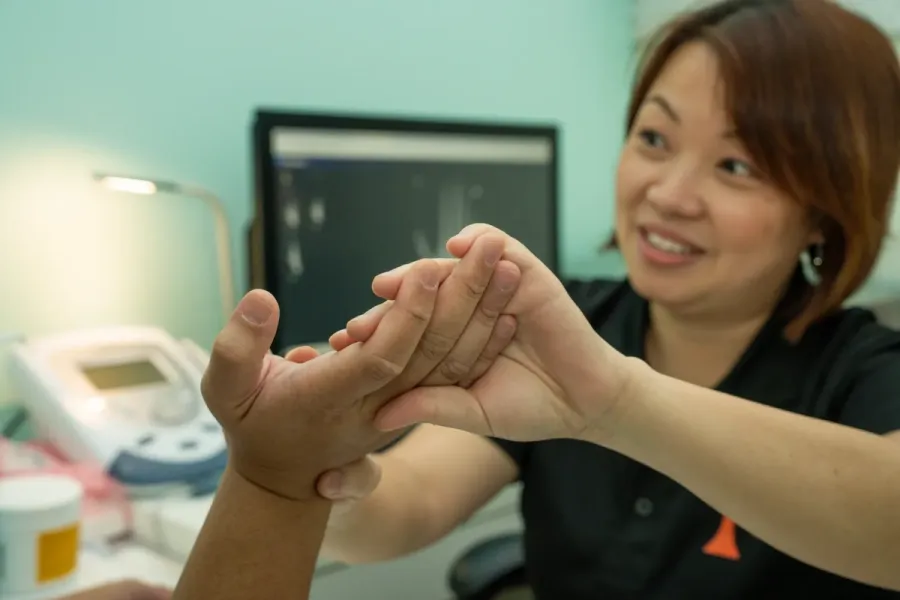
-
Hip Pain Physiotherapy
-
Hip Pain Physiotherapy
Hip pain can be caused by many factors, such as hip fractures, hip joint injuries, muscle strains or contusions, nerve irritation and arthritis or osteoarthritis.
Our primary concern is ruling out and managing any underlying undiagnosed issues, such as infections or cancerous cell growths that may cause pain - if in doubt, please immediately see your doctor.
If it's not severe, it's most likely a non-fracture musculoskeletal condition. In this case, with regular physiotherapy, we can help to build and restore your hip joint range of motion, hip strength and normal walking patterns!
LEARN MORE Book an appointment today
-
Knee Pain Physiotherapy
-
Knee Pain Physiotherapy
Knee pain is a common complaint for many people (we should know - we treat many knee pain patients at our physiotherapy clinics!).
There are a variety of modalities to treat knee conditions, ranging from sports massage therapy sessions and joint mobilisation to shockwave therapy and radiofrequency INDIBA physiotherapy.
Patients may also benefit from regular core strengthening exercises, including clinical Pilates and acupuncture therapy for pain management.
LEARN MORE Book an appointment today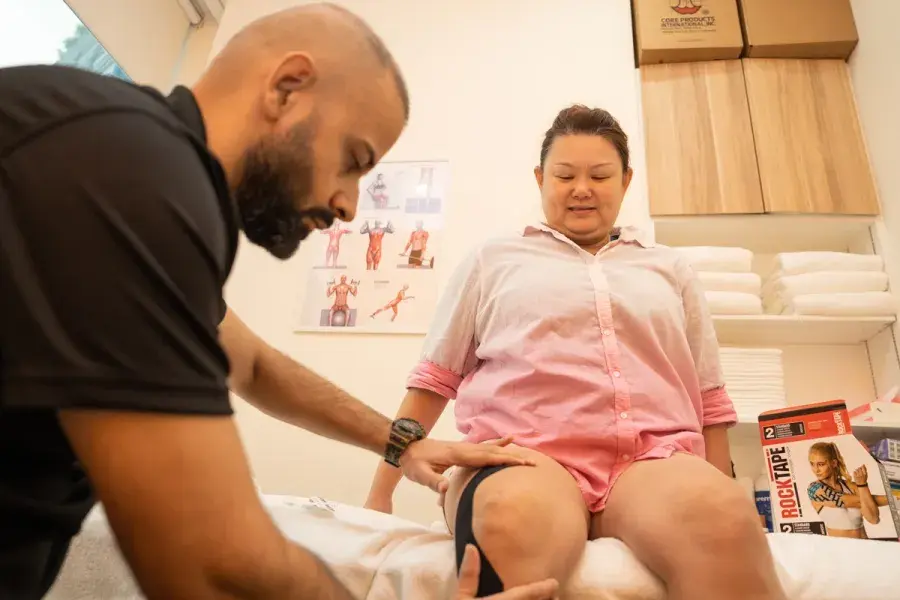
-
Foot Pain Physiotherapy
-
Foot Pain Physiotherapy
Foot pain is a common problem, with telltale symptoms such as burning pain, swelling and numbness.
Foot pain can be caused by conditions or injuries such as sprains, tendonitis and bone spurs. Most cases of foot pain will settle down with careful and early foot physiotherapy management.
LEARN MORE Book an appointment today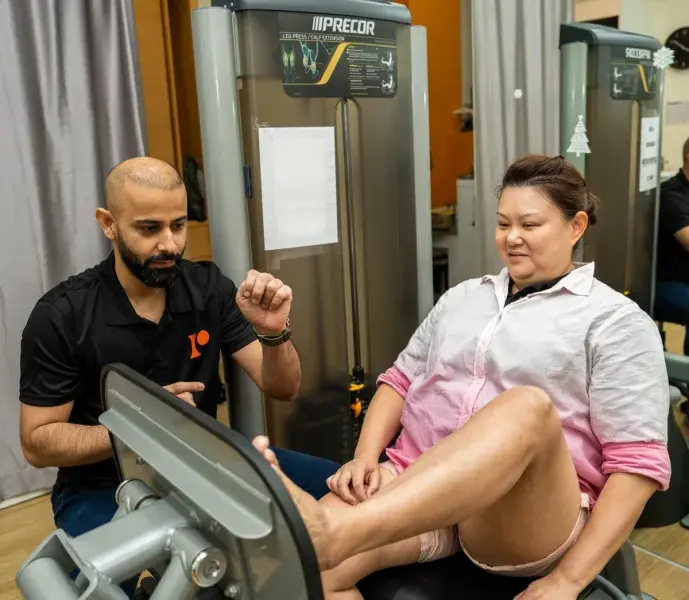
-
Tendon Pain/Tendinopathy Physiotherapy
-
Tendon Pain/Tendinopathy Physiotherapy
Tendon pain or Tendinopathy usually causes pain, stiffness, and loss of strength in the affected area.
Physiotherapists can typically rehabilitate injured and painful tendons quickly and effectively. However, a percentage of tendinopathies can take months to treat.
Every tendon injury, pain and Tendinopathy is different, so our consultation sessions are crucial to providing the best tailored holistic care.
Book an appointment today
-
Women's Health Physiotherapy
-
Women's Health Physiotherapy
The Phoenix Rehab Group's Women's Health Physiotherapy division comprises passionate specialists managing pre- and post-pregnancy and delivery-related musculoskeletal conditions and pains.
Our women's health therapists will apply gentle clinical treatment approaches to help improve and restore the movement and stability of your spine, pelvic girdle and lower back, boost pain relief, decrease muscle spasms and improve strength and stamina.
Book an appointment today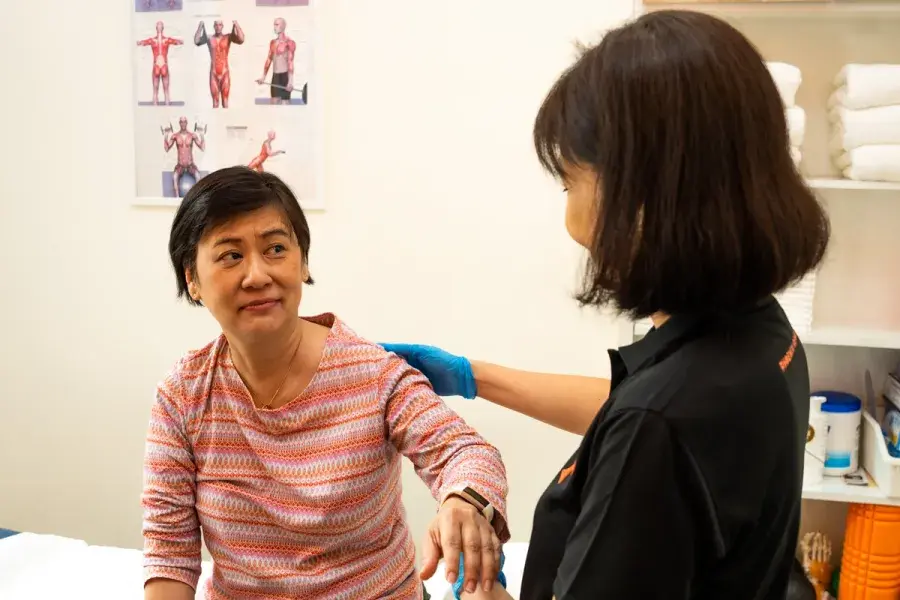
-
Post-surgery Physiotherapy
-
Post-surgery Physiotherapy
Post-surgery rehabilitation is a complex and delicate process that requires skilled training and experience.
After undergoing orthopaedic surgery to reduce pain and movement limitations, you'll require exercises and progression to regain your strength, flexibility, movement and function fully.
However, restoring optimal physical function and strength depends on the person's level of active participation during rehabilitation.
Furthermore, you can count on us to liaise with your surgeon to determine specific requirements and ensure optimal supervision and support on your recovery journey.
Book an appointment today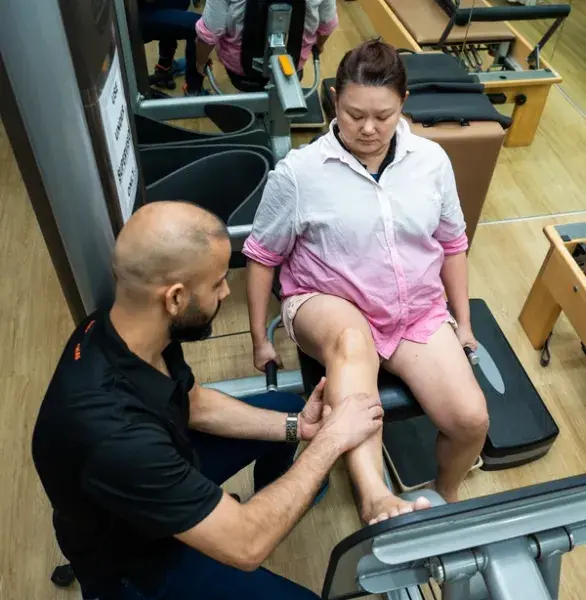
-
Sports Physiotherapy
-
Sports Physiotherapy
Our sports physiotherapists are trained to develop customised rehab programs, using specialised assessments to diagnose and treat various sports injuries.
You will be under the care of your sports physiotherapist, who will regularly evaluate your progress to have you return swiftly to the sports you love.
LEARN MORE Book an appointment today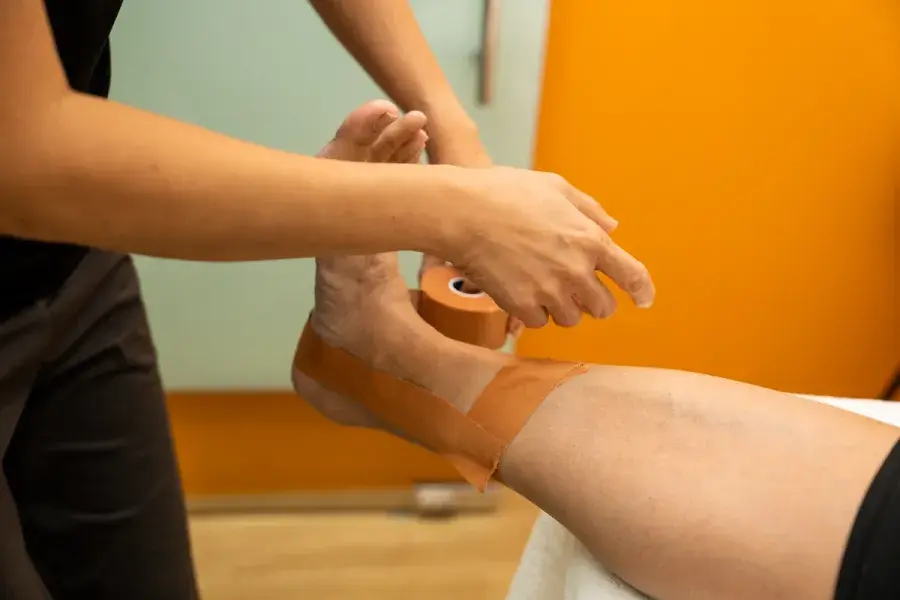
-
Pilates
-
Pilates
Every clinical Pilates programme is customised for every individual - there is no one-size-fits-all. That said, each programme features one of these main Pilates types:
Clinical Pilates: Combines Pilates fundamentals with Physiotherapy research and education, particularly emphasising the activating, strengthening, and improving the flexibility of our core muscles.
Reformer Clinical Pilates: Treats a full range of orthopaedic, sports conditions and injuries to accelerate your return to work, sports, and life safely.
LEARN MORE Book an appointment today
-
Dry Needling Physiotherapy
-
Dry Needling Physiotherapy
Dry needling is a technique used by physiotherapists to treat muscle pain and tightness, where a small needle is inserted into the muscle to create a 'local twitch response'.
This sets off the correct physiological response to treat pain, which may be felt as a slight cramp or muscle contraction of a very short duration (usually 1-2 seconds).
It is important to note that dry needling, a Western treatment, is not Acupuncture, which is only performed by qualified Traditional Chinese Medicine (TCM) practitioners.
Book an appointment today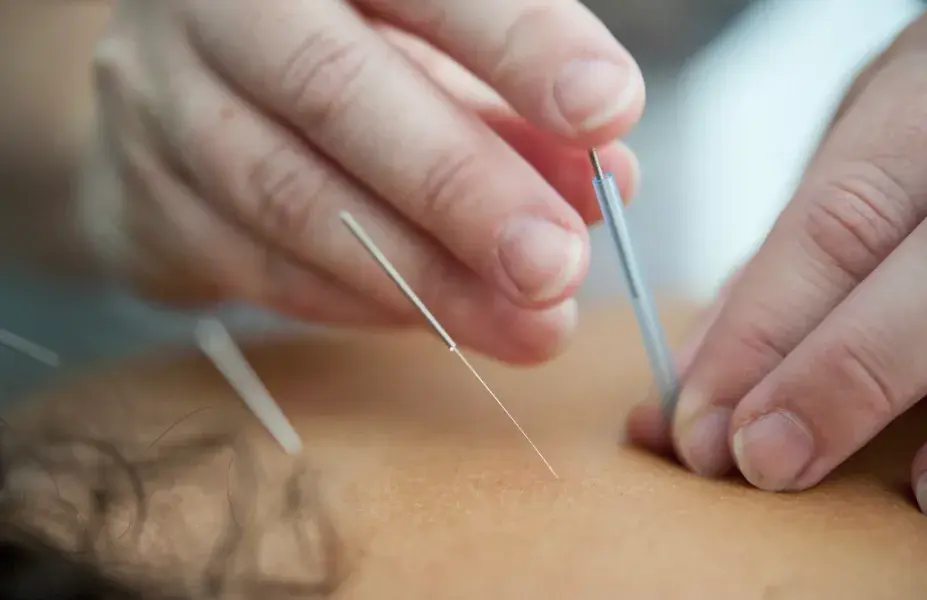
-
Personal Training
-
Personal Training
Our personal training programmes utilise science-based methods and a holistic approach to help you meet your health and fitness goals at any age, even if you have had past old injuries, health conditions or struggles!
We currently offer Fat Burning Programme, Muscle-building Programme and Sports Performance Programme.
The right program for you depends on your schedule, health and fitness goals, and medical history.
Book an appointment today
-
Ergonomics Physiotherapy and Repetitive Strain Injury Prevention
-
Ergonomics Physiotherapy and Repetitive Strain Injury Prevention
Did you know that Repetitive Strain Injuries (RSIs) account for 40.9% of the patients treated in our physiotherapy clinic?
RSIs refer to a range of neck, shoulder, arm, wrist and hand disorders that can be caused or made worse by work.
The best way to treat RSIs is to prevent them, saving companies and employees time, effort and costs. We will be most glad to assist you in building a positive and healthy work environment.
Thus, we provide Phoenix Rehab Human Factors Solutions, including Ergonomic Workstation Evaluation, Comfort Level Survey, Talks, Workshops and Group Training.
Book an appointment today
-
Office Ergonomics Advice, Talks and Workshops
-
Office Ergonomics Advice, Talks and Workshops
Work-related musculoskeletal disorders (WMSD) are usually seen in the hand, arm, shoulder, neck, thoracic and lower back.
In fact, WMSDs are one of the most frequently reported causes of lost or restricted work time; having healthy and pain-free employees translates to having a more productive and profitable business.
We can help by providing you with a tailor-made Corporate Ergonomics Intervention Programme that includes
-Identification of Ergonomic Hazards
-Good/Practical Advice
-Exercises Stretches, or Therapeutic tools
-Adjustments and Recommendations
-a Report from our qualified, AHPC-recognised physiotherapists
Book an appointment today
-
Aquatic/Hydrotherapy
-
Aquatic/Hydrotherapy
Aquatic therapy is a physical medicine and rehabilitation speciality conducted in a pool or other aquatic environment under the supervision of a trained physiotherapist.
In Singapore, it is covered by many health insurance providers due to the personalised nature of the treatment.
LEARN MORE Book an appointment today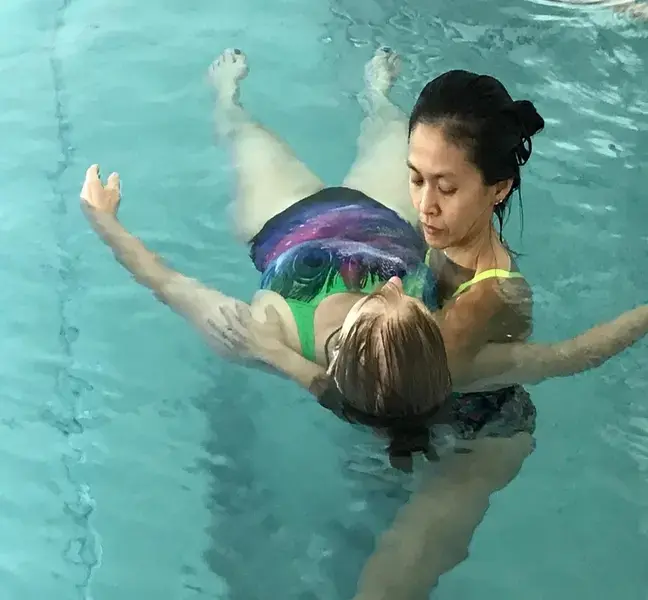
The Phoenix Process: Feel Reborn with Our Tailored Physiotherapy in Singapore
Step 1: Initial Consultation
At Phoenix Rehab, we prioritise creating a relaxed, patient-centred environment.
We'll work with you to address your symptoms and concerns, ensuring that you fully understand your condition before proceeding with treatment; we prioritise you making an informed decision.
Step 2: In-depth Review
Our friendly physiotherapists will conduct an in-depth review of your medical history to fully understand your symptoms, lifestyle, and health goals.
This is a crucial step in forming a customised treatment plan that accounts for the patient's past and current medical conditions, underlying issues, or potential problems that may arise in the future.
Step 3: Assessment
Based on your review, we'll conduct clinical tests and physical assessments to understand the severity of your condition.
This aids us in ruling out potential underlying causes, injuries or safety concerns and provides an accurate diagnosis. Our clinic prioritises safe and effective treatments that tackle health issues without triggering adverse side effects.
Step 4: Treatment
We'll discuss a customised treatment plan to help you reach your health goals based on our findings. Most patients will receive physiotherapy treatment within the same session.
Naturally, our expert Physiotherapists will conduct regular observations during each of your follow-up sessions, allowing us to track your progress and adjust the intensity of our treatments accordingly for a speedy recovery!

The Physiotherapy Clinic You Can Trust
Our experienced physiotherapists are experts in assessing, diagnosing, prescribing, and treating movement and physical injuries, regardless of the cause of the pain.
Certified & Registered Physiotherapists with the Allied Health Professionals Council (AHPC)
Decades of Combined Experience and Expertise Across a Variety of Conditions
Locally & Internationally Trained in Various Treatments, Techniques & Technologies
Reclaim your mobility, regain your strength, and rediscover the joy of pain-free movement with our exceptional Physiotherapy services.
Whether you're dealing with injuries or musculoskeletal conditions, our expert physiotherapists help you regain pain-free movement, enhance function, and improve your overall quality of life.
We are committed to staying at the forefront of advancements in the field, ensuring you receive the most effective and innovative treatments.
Don't let pain and limitations hold you back any longer.
Take the first step towards a healthier, more active lifestyle by scheduling a consultation with our experienced team at Phoenix Rehab today!
Learn more about Physiotherapy
We are a bone, muscle, joint, tendon and ligament physiotherapy and hand therapy clinic in Singapore, operating in Novena and Tampines. We offer a unique integrated and multi-specialty approach to pain and injury rehabilitation with expert physiotherapy, hand therapy, TCM, massage, alternative therapies and rehabilitation technologies.
 Whatsapp us now
Whatsapp us now